Capell Lab
The Capell Lab seeks to understand how epigenetic and chromatin regulatory mechanisms contribute to disease. By combining the incredible accessibility of human skin with the most cutting-edge epigenetic and genome-wide techniques, we aim to identify novel targets to treat disease.

Ellebrecht Lab
The combined focus of the Ellebrecht lab is to understand immune cells in the context of autoimmunity and manipulate them for use as precision cellular immunotherapies. We are particularly fascinated with immune cells and their ability to remember: if we are exposed to a pathogen a second time, our immune system responds quicker and more vigorously than the first time around. Our research aims to elucidate the mechanisms behind how and when specialized human T lymphocytes, that are used to treat patients or reside in specific organs, commit to long- or short-lived cell fates. We believe that science is centered on pushing the boundaries of knowledge and technology. To that end, we employ single cell multiomics to dissect fate decisions in human immune cells; our ultimate goal is to uncover the intricacies of autoimmunity and translate our findings to engineer next generation immunotherapies.
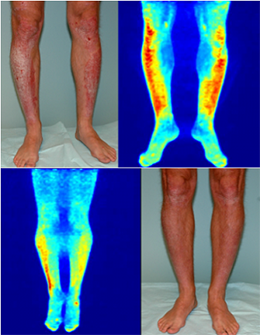
Gelfand Lab
The Gelfand Clinical Research Lab designs and conducts interventional and translational clinical trials as well as observational and pharmacoepidemiological studies in common and rare skin diseases. We aim to improve psoriasis patient outcomes in the skin and joints, while lowering the risk of diabetes, cardiovascular disease and mortality. In addition with our new LITE Study (Light Treatment Effectiveness Study), we hope to narrow the gap in knowledge for patients, dermatologists, and payers on the effectiveness of home-based versus office-based phototherapy through the design and conduct of a pragmatic trial in 1050 patients across the US.

Grice Lab
The skin is a formidable barrier and the first line of defense against the external environment. The skin is also colonized with microbial communities, which we hypothesize have critical functions in cutaneous health and disease. These functions may include but are not limited to colonization resistance to block invasion by opportunistic or pathogenic microbiota and regulation of immunity and inflammation. Various cutaneous disorders and infections are hypothesized to in part result from dysregulation of microbiota-host interactions. The Grice lab applies a variety of different approaches, model systems, and human tissues and isolates to elucidate mechanisms regulating such interactions.
Currently, research in the Grice laboratory is divided into the following focus areas:
(1) Skin microbiome regulation of epithelial defense
(2) Microbial regulation of tissue repair and inflammation in chronic wounds
(3) Skin microbiota-driven mechanisms of colonization resistance to pathogens
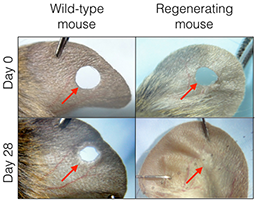
Leung Lab
The Leung lab uses molecular genetically based techniques to functionally dissect the mechanisms driving mammalian tissue regeneration and inflammatory skin diseases, in both mouse and humans. We aim to develop new therapeutic approaches in regenerative medicine.

Margolis Lab
Dr. Margolis’s research work is focused on dermato-epidemiology and, more specifically, the epidemiology and treatment of chronic wounds, atopic dermatitis, and acne. Dermatologic illnesses are highly prevalent and tend to be chronic. For example, atopic dermatitis affects about 10% of our population and tends to wax and wane over a lifetime. His research awards have been focused on the treatment of patients with chronic cutaneous wounds, such as diabetic foot ulcers, the prevention of chronic cutaneous wounds, the treatment of atopic dermatitis, the genetic variants of atopic dermatitis, cardiovascular disease and psoriasis, the effect of chronic antibiotic exposure in patients with acne, and the effectiveness of acne therapies.
Ridky Lab
The Ridky Lab uses genetically-defined, engineered epithelial tissues as an experimental platform to study pathways driving human cancer initiation, tumor-stroma interaction, invasion and metastasis, maintenance of cancer stem cells, and regulation of skin pigmentation.
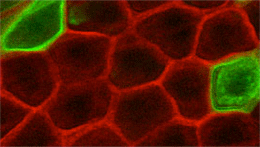
Rompolas Lab
In our laboratory we use advanced microscopy and mouse genetic tools to study the biological basis of skin regeneration. Our goal is to understand the mechanisms that stem cells employ to maintain and replenish the skin throughout life and to uncover which of these processes, when deregulated, are responsible for the emergence of disease.
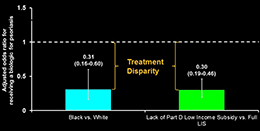
Takeshita Lab
Our research group seeks to identify, understand, and eliminate health and health care disparities in dermatologic diseases. We use mixed (quantitative and qualitative) methods to study and address disparities in chronic inflammatory skin diseases (e.g., psoriasis, atopic dermatitis) with an aim to achieve health equity in dermatology.
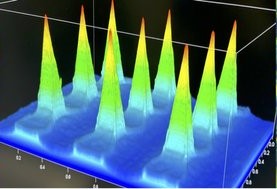
Wang Dermatologic Bioengineering Laboratory
The Dermatologic Bioengineering Laboratory is located in the Department of Dermatology at the Perelman School of Medicine of the University of Pennsylvania. We are a thriving community of expert clinicians, biologists, engineers, and chemists with a shared goal of solving clinical dermatology challenges that affect human health. We do this by identifying gaps in clinical care, overcoming these gaps with bioengineering, and then translating our advances back into the clinic. Specific interests in our laboratory include biomaterials, hydrogels, polymer chemistry, polymer-drug conjugates, drug delivery, biofabrication, tissue engineering, diagnostics, and therapeutic development. Our clinical interests include autoimmune skin disease, wound healing, scarring, calcifying disorders, and hair loss.
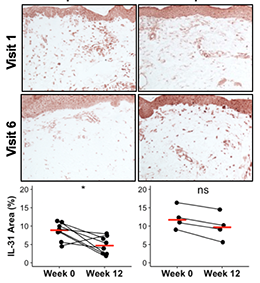
Werth Lab
The Werth lab uses cell immunophenotyping and gene signatures to determine the heterogeneity of response to treatment in autoimmune skin diseases. This heterogeneity provides insights into disease pathogenesis, including symptoms such as itch (see image). We also study the effects of ultraviolet light in photoaging. We have developed disease severity indices used widely in international multicenter clinical trials in autoimmune skin diseases.
